By Dr. Peter Klapper Ph.D.
Living with psoriasis can be a struggle for many people—especially before finding a diagnosis. Many times, people assume that the dry and patchy skin is a result of dry skin or eczema. They apply moisturizer, see no result, and feel frustrated as it begins to appear in more areas on the body. So, if there isn’t a psoriasis eczema rash, what exactly is psoriasis? For insights into personal experiences, read Living with Plaque Psoriasis.
What is Psoriasis?
Psoriasis is a chronic autoimmune skin condition that affects 125 million people worldwide. It is a complex disease with a range of symptoms and triggers that can significantly impact a person's quality of life. Many wonder, is psoriasis contagious? Fortunately, it’s not. It is a skin disorder characterized by the rapid growth of skin cells. Normally, skin cells go through a cycle of growth and shedding over several weeks.
However, in individuals with psoriasis, this process is accelerated to just a few days, causing an accumulation of thick, scaly patches on the skin's surface. To learn about natural treatment options, consider our Top 10 Homeopathic Ingredients for Psoriasis. If you're experiencing scalp issues, our article on Scalp Psoriasis might be helpful.
As with any physical ailment, this disease not only affects individuals from the discomfort their experiencing but can influence a person’s mental state as well. Due to the scaly patches on the skin, a person may feel embarrassed or worried what others think. Frustration may occur by the persistent symptoms of psoriasis such as the itching and flaking that comes with flare-ups. A person may also feel isolated, stressed, or even depressed due to withdrawing from activities and dealing with the emotional toll that can come from psoriasis.
Luckily, every August during “Psoriasis Awareness Month,” various organizations and healthcare professionals aim to educate the community about the impact on individuals' lives and the importance of research and support for those affected by psoriasis.
What Are the Symptoms of Psoriasis?
As with any disease, symptoms can vary, but with psoriasis most common symptoms include:
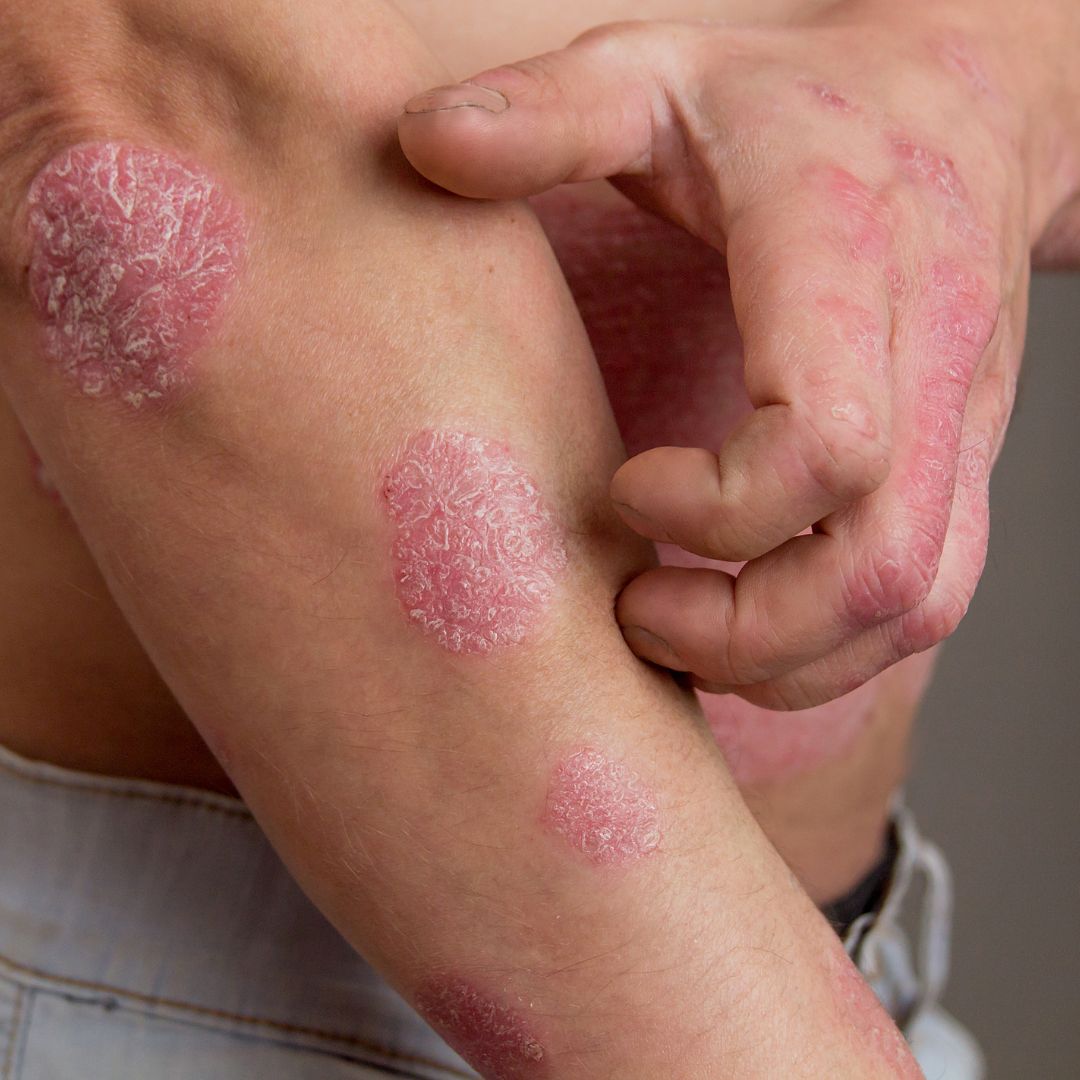
Red and Inflamed Skin Patches: The most common symptom of psoriasis is that the affected skin areas become red and inflamed, often covered with silver or white scales. This distinctive appearance helps differentiate psoriasis from other skin conditions.
Dry, Cracked, and Painful Skin: The skin patches may become dry, rough, and prone to cracking, which can be painful and cause discomfort. Especially if they begin to bleed.
Itching and Burning Sensations: Psoriasis can be intensely itchy, leading to scratching, which can further irritate the skin and trigger more flare-ups.
Thickened and Pitted Nails: Psoriasis can affect the nails causing them to become thick, pitted, and discolored. In severe cases, nails may loosen from the nail bed.
Swollen and Stiff Joints: Around 30 percent of people with psoriasis develop psoriatic arthritis, which causes joint pain, swelling, and stiffness. Psoriatic arthritis can severely impact joint function and mobility.
Triggers of Psoriasis
Triggers of psoriasis can vary from person-to-person. For some, a change in the weather can create a flare-up and others it could be as simple a bug bite. While the exact cause of psoriasis remains unknown, it is important to understand your triggers so that you can better manage when your psoriasis makes an appearance.
Some common triggers include:
Stress: If your stress isn’t managed, it can weaken the immune system and trigger psoriasis symptoms. Which is, of course, hard if you’re already stressed from the presence of your psoriasis.
Infections: Bacterial or viral infections, such as strep throat, can cause psoriasis to worsen. Being proactive when you get sick can help keep your psoriasis at bay.
Weather Conditions: Cold, dry weather may dry out the skin and worsen psoriasis symptoms.
Medications: Certain medications, such as lithium, beta-blockers, and antimalarial drugs, can trigger or aggravate psoriasis in some individuals. When in doubt, let your healthcare provider know if you have psoriasis, so they can be aware when prescribing you new medications.
Injury to Skin: Injuries to the skin, such as cuts, burns, or bug bites, can trigger the development of psoriasis lesions in the affected area otherwise known as the Koebner phenomenon.
Smoking and Alcohol: Both smoking and excessive alcohol use can not only increase your risk of developing psoriasis but worsen an existing condition.
Hormonal changes: Fluctuations in hormones, such as during pregnancy or menopause, can influence psoriasis symptoms.
Obesity: People who are overweight or obese may experience more severe psoriasis symptoms.
Types of Psoriasis
Psoriasis can look different for everyone. So much so that there are various types of psoriasis each presenting with unique characteristics that require a different treatment approach. The most common types of psoriasis include:
Plaque Psoriasis is the most common type, accounting for about 80-90% of all cases. It appears as raised, red patches covered with silvery scales, often occurring on the scalp, knees, elbows, lower back, and palms.
Guttate Psoriasis is characterized by small, drop-like lesions that are thinner than the typical plaques seen in plaque psoriasis. It often develops after a bacterial or viral infection and is more common in children and young adults.
Scalp Psoriasis affects the scalp and can cause red, scaly patches, itching, and flaking, often resembling dandruff.
Nail Psoriasis affects the nails, leading to changes like pitting (small depressions), discoloration, crumbling, and detachment of the nail from the nail bed.
Erythrodermic psoriasis is a severe and rare type of psoriasis that affects large areas of the body. It causes intense redness, shedding of skin, and can be life-threatening due to potential complications related to fluid loss and temperature regulation.
Psoriatic Arthritis is a type of inflammatory arthritis that occurs in individuals who have psoriasis. It primarily affects the joints, leading to pain, tenderness, and swelling. Psoriasis arthritis symptoms can involve any joint but commonly affects the fingers, toes, knees, ankles, and lower back.
Treatment Options
Unfortunately, at present there is not a cure for psoriasis. It’s a chronic condition in which individuals must learn to adapt. However, there are various treatment options that can manage symptoms from a flare-up and greatly improve quality of life. Speak with your healthcare provider to see if the following treatments may work for you.
Topical Creams and Ointments: Creams, ointments, and lotions containing corticosteroids, retinoids, or vitamin D analogs can help reduce inflammation and scaling. These are often used for mild to moderate psoriasis.
Phototherapy: Phototherapy, a treatment that uses controlled amounts of natural or artificial ultraviolet light to slow down cell turnover and ease symptoms, is beneficial for moderate to severe psoriasis.
Oral Medications: Prescribed by your doctor, these psoriasis medications work by targeting different aspects of the immune system and inflammatory pathways involved in psoriasis.
Biologic Drugs: While considered a newer class of medications, biologic drugs target specific components of the immune system that are involved in the inflammatory process that generates psoriasis. Biologic psoriasis medications are typically administered via injection or infusion and are often reserved for moderate to severe cases that have not responded well to other treatments.
Natural Treatments: If you choose to go the natural approach, Forces of Nature’s Psoriasis Treatment rejuvenates damaged skin without steroids or side effects making this a safe choice for your body, scalp, and overall health. Our treatment contains anti-inflammatory certified organic plant extracts that strengthen the system to quickly soothe and relieve psoriasis while working with your body’s natural immunity.

Knowing that you will forever have a chronic condition such as psoriasis can be hard to swallow. It is both physically and emotionally exhausting, especially if it takes a toll on your lifestyle. However, once an individual has chosen to accept and acknowledge that this is their new normal, real change can happen. Especially if you make changes to your lifestyle to help prevent future flare-ups. Those may include:
Maintaining a healthy diet
A balanced and nutritious diet can play a significant role in managing psoriasis. Incorporate plenty of fruits, vegetables, whole grains, lean proteins, and healthy fats into your meals.
Avoiding Smoking and Alcohol Consumption
Similar to maintaining a healthy diet, you should also avoid alcohol and smoking. Particularly because smoking and excessive alcohol consumption have been linked to an increased risk and severity of psoriasis.
Managing Stress Levels
As we discussed above, stress is a trigger. By managing it you can prevent future flare-ups. If you aren’t already, practice mindfulness techniques such as meditation, yoga, deep breathing exercises, or even taking a bubble bath at home to melt away the stressors of the day.
Practicing Good Skincare Habits
Whether that looks like being proactive with sunscreen or avoiding picking at affected skin areas, skin care is important. Be sure to moisturize regularly to help to prevent dryness and reduce itching. That said, make sure to use fragrance-free, hypoallergenic moisturizers to avoid any potential skin irritations.
Stay Consistent
By keeping consistent with your lifestyle changes and staying on top of your treatment plan, you can work to minimize potential flare-ups. However, it is important to note that what works for one person may not work for another, so keep testing out changes that make a noticeable difference.
Moving Forward
As with any condition that is chronic, it’s important to lean on your community for support. Whether that looks like joining support groups or online communities, educating your family and friends, or finding guidance from healthcare professionals, all can help you adjust to living your new normal.
Remember, managing psoriasis is possible, and with the right approach, you can lead a fulfilling life despite the challenges posed by this condition.